Dislocations and leg fractures are some of the most common skydiving injuries, and ankles are the most frequently injured joints. The incidence of ankle injuries ranges from 1 to 4.5 per 1,000 jumps, and ankles account for 30-60% of all parachuting-related injuries. Injury rates are higher for inexperienced jumpers, at 6 to 7 injuries per 1,000 jumps.
A Danish study of amateur sport jumpers reports that of 110,000 jumps recorded over five years, 155 (0.14%) involved injuries that required medical treatment. Of these, 98 of 155 (63%) were fractures, with nearly half being ankle fractures. A Swedish study of sport parachutists concluded leg trauma accounted for 51% of reported injuries. In both studies, injuries occurred during landing 83-90% of the time. Terrain landing conditions matter a great deal in injury rates, with the ideal landing area being soft earth or sandy soil. Experience also matters, with injury rates nearly three times higher for beginners compared to advanced flyers, and six times higher for students compared to licensed skydivers.
Poor body positioning contributes to many landing injuries with inexperienced jumpers. Beginners tend to stiffen their bodies as the ground gets closer. They often approach landing with legs separated and one leg extended downward. This leads to one foot hitting the ground first and transmitting that sudden-impact force to either the ankle or knee, depending on the angle of the foot and leg. Ouch! A study of the parachute landing fall found that inexperienced parachutists tend to land heel first and straighten the hips and knees as their feet hit the ground, compared to experienced parachutists who tend to land with toes first (on both feet) while flexing their hips and knees when their feet strike earth, reducing that sudden-impact force to their knees and ankles.
What are the common ankle injuries in skydiving?
Ankle Sprains and Strains
A sprain is defined as an injury to a ligament (tissue connecting two bones). In contrast, a strain is an injury to a muscle body or a tendon (tissue connecting muscle to bone). The most common ankle sprain (70-90% of all sprains) is injury of ligaments on the outside of the ankle by rolling the foot inward. There are three ligaments on the outside of the ankle and they are often damaged in a predictable sequence as trauma force increases. The ligaments on the inner side of the ankle are far stronger and injure less frequently. Injuries to these ligaments generally occur with rolling of the foot outward.
Sprains are classified from Grades I through III. Grade I is ligament stretching, which causes pain but still allows walking. Grade II is a partial ligament tear, which causes considerable pain and swelling that prevents walking. Grade III is a complete ligament tear, which results in severe pain, instability and inability to stand or walk. Importantly, a previously sprained ankle is five times as likely to injure again compared to a non-injured ankle.
Ankle Fractures
Ankle fractures (aka broken bones) can range from small, chip fractures similar to those sometimes found in ankle sprains, up to multipart, unstable fractures. Think about the ankle as a tripod, with two points of the tripod as the bony bumps on either side of your ankle and the third point of the tripod as the back of the ankle, which you can’t feel because the Achilles tendon covers it. (See Figure 1.) It is more common to break the bony bumps on either side of the ankle compared to the back one. As might be expected, the more of these you break, the less stable your ankle becomes. Breaking all three bones is called a “trimal fracture.” These breaks usually occur from injuries that cause the foot to fold under, but more severe injuries come from a sudden-impact force pushing your foot up and rotating it out. (See Figure 2.) One of the most severe injuries is called a “Pilon fracture,” when impact force literally drives the foot bones up into the ankle, causing multiple breaks (See Figure 3.) Imagine a firecracker in your ankle joint exploding; this is almost what it looks and feels like. Any break in the skin or cuts over a fracture is bad and greatly increases the risk of infection and complications.
Ankle Dislocations
Nearly all ankle dislocations have an associated ankle fracture; pure ankle dislocations are rare. (See Figure 4a.) These typically occur when a force is applied directly to the bottom of the foot up through the ankle. Imagine jumping from a chair to the floor and feeling the impact force on the soles of your feet as you land. This force can cause the foot to shift and dislocate either forward, backward or sideways relative to the lower-leg bones. Backward dislocations are most common. (See Figure 4b.)
Skin tenting—when dislocated bones create a lot of pressure and act like tent poles to stretch the skin out—often occurs with dislocations. This is bad news and can quickly kill that skin, exposing the dislocated joint or broken bone to bacteria and increasing the risk of infection. Fractures with dislocations tend to have worse function in the future compared with fractures alone. Any loose bone chips that remain in the joint after reduction also greatly increases the risk of future arthritis and worse function.
Achilles Tendon Rupture
The Achilles tendon (See figure 1) is the largest and strongest tendon in the body. It attaches the calf muscle to the heel bone and allows us to perform functions such as pointing and standing on the toes. A rupture typically occurs when the toes (and tip of the foot) experience a strong, sudden force that bends toes up very quickly and causes the tendon to tear off at the heel bone. This is often described as hearing or feeling a “pop” at the back of the leg, suddenly not being able to walk on that foot and feeling like you were kicked in the back of the ankle. This occurs frequently in running or jumping sports. In skydiving, the greatest risk is during landing or running out a landing, as your toes are forced upward when you touch down. An Achilles tendon rupture is more common in men and can occur even with lower impact injuries after the age of 40. There are also certain medications (e.g., antibiotics) that can increase the risk of this injury. Make sure to ask your doctor about this if starting a new antibiotic.
Arthritis
While not technically an injury, arthritis can greatly affect the ability to stay active in this sport that we love. Luckily, ankle arthritis is rare, and the diagnoses of arthritis on X-rays does not seem to match reported ankle pain. There is a higher rate of arthritis among those with previous ankle fractures, especially if the break extended into the joint.
What can I do to help someone with an ankle injury?
For anyone suspected of having an ankle injury, field management is to first stop any active wound bleeding and then stabilize the foot to prevent movement. For a suspected sprain, first elevate the foot (ideally above the heart), wrap with an ace bandage to help control swelling and apply an ice pack. For a possible fracture, use a rigid splint to prevent the foot from moving. As discussed in the article “Tools of the Trade: Drop Zone Medical Kits” (Parachutist, February 2023), the best splint is an aluminum splint (i.e., SAM splint). You can place this under the bottom of the foot, where it then extends up behind the ankle and lower leg, and strap it to the foot with an ace bandage. If you have a second splint, place it side-to-side around the ankle and under the foot like a horseshoe to provide extra stability. (See Figure 5a/b.) If you don’t have a SAM splint available, fashion an improvised splint out of cardboard or other rigid material, or pack clothes around it to prevent movement.
For any bleeding wound, use direct pressure with clean gauze or a clean cloth. Broken bones tend to ooze a lot and may continue to bleed until the fracture is reduced. If there is a large amount of bleeding or you cannot control it with direct pressure, don’t hesitate to apply a tourniquet above the wound (at least one to two hand widths above the fracture).
When should I be worried or seek medical attention if I am injured?
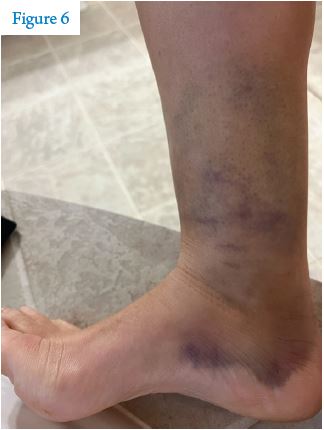 If it looks jacked up (i.e., you have an obvious break or dislocation), get it checked out. For those “rolled ankles” or hard landings that you might just walk off, go in for an X-ray if your ankle is tender when you push on the bony knobs that stick on either side or if you can’t walk on it due to pain (either immediately or the next day). Bruising is not necessarily indicative of injury severity. Sometimes significant bruising all over the ankle needs nothing more than ice and an ace wrap. (See Figure 6.)
If it looks jacked up (i.e., you have an obvious break or dislocation), get it checked out. For those “rolled ankles” or hard landings that you might just walk off, go in for an X-ray if your ankle is tender when you push on the bony knobs that stick on either side or if you can’t walk on it due to pain (either immediately or the next day). Bruising is not necessarily indicative of injury severity. Sometimes significant bruising all over the ankle needs nothing more than ice and an ace wrap. (See Figure 6.)
What can I expect at the emergency department, and what is the simplified long-term management of ankle injuries?
Ankle Sprain
In case of an ankle sprain, you may be placed in anything from an elastic bandage (ace wrap), removable air cast, walking boot or temporary splint. The higher the grade of the sprain, the more rigid immobilizer you will need. For less-severe injuries, a combination of rest, ice or cold water immersion, compression with an ace wrap and elevation (above your heart) will likely be sufficient. You should use ice or cold-water immersion for no more than 15 - 20 minutes every two to three hours for the first 48 hours or until swelling is reduced (whichever comes first). Acetaminophen (Tylenol) is good for pain relief, and use NSAIDS (Motrin or Advil) for both pain and to help reduce inflammation.
Semi-rigid ankle support braces will lead to a quicker return to the sport, but lace-up splints or compression wraps are better to prevent swelling. A combination of both (air cast when walking or with activity and ace wrap with resting) is likely the best answer. Ace wraps are best applied in a figure-eight pattern to maximize stability. For severe sprains, surgery may be needed to prevent recurrence and has been shown to decrease instability.
Physical therapy can help you return to the sport more quickly and reduce risk of recurrence. You should start a combination of range-of-motion exercises along with strength exercises as early as pain and swelling allow. A great resource for these can be found at orthonc.com/uploads/pdf/Ankle_Foot_AROM.pdf. You should wear your splint or brace during early exercise. A minimum of three weeks of rehab is recommended; however, it may take several months to return to full activity without pain in more severe sprains. You can return to full sport activity when the swelling and pain have resolved and you can complete sport-specific movements without instability, pain or next-day swelling. A good test of the joint is to try a balance test (stand on one foot for at least 10 seconds), star test (stand on injured foot and extend other foot as far as possible to touch eight points around your body in a star pattern) and a side-hop test (20 side-to-side hops at least 30cm apart).
Ankle Fracture
The emergency department may treat small-chip fractures just like sprains. More severe fractures often require setting or reduction (under sedation) in the emergency department and placement in a splint until an orthopedic surgeon evaluates it. Many people with awful-looking fractures are surprised when they can be sent home after a good reduction in the emergency department. The splint helps keep broken bones from moving around, which decreases pain a lot, and elevation plus painkillers will generally lower remaining pain to a tolerable level. Many fractures will eventually require surgery (See figure 8), but most surgeons recommend waiting until swelling goes down to minimize complications. So don’t be 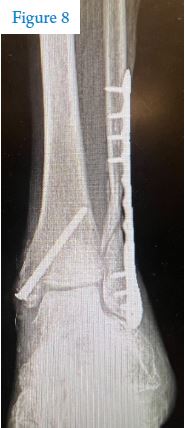 surprised if surgery is a number of days out from the injury.
surprised if surgery is a number of days out from the injury.
Fractures with associated skin tears or cuts with exposed bone are a different story. These generally require admission to the hospital for IV antibiotics and more immediate surgery to decrease risk of infection. Likewise, if the emergency physician is unable to set the bones in the correct position, or if there is concern over a nerve being trapped or damaged (if part of your foot is numb), you will probably be admitted for surgery.
Ankle Dislocation
This will always require reduction in the emergency department under sedation, and you will be placed into a rigid splint afterward. Let the doctor immediately know if you cannot feel any part of your foot either before or after the reduction, as this may indicate damage to the blood vessels or nerves. Nearly all of these injuries require surgery, and post-reduction management is similar to that of ankle fractures.
Achilles Tendon Rupture
The emergency department places these injuries in a splint molded so the foot is pointed down and out. Early follow up with orthopedic surgery (within one week) is important to discuss surgery versus management using only a cast. Younger or more active patients have a higher chance of being recommended for surgery. Often, the outcome of keeping the leg in a cast for a couple of months is just as good as with surgery, and there is no difference in repeat injury rates, flexibility or return to level of sport. Unfortunately, you will likely be grounded for almost five months, regardless of treatment. Physical therapy is a must, with early range-of-motion exercises once the cast is removed and strength exercises starting roughly three months later.
Are there ways to prevent ankle injuries?
What about wearing braces to prevent an injury? This can actually work! Most of this information comes from military parachutists, who have used rigid, outside-the-boot braces to help prevent ankle injuries when landing. Studies show that rigid braces (similar to air casts) help prevent the ankle from turning inward when landing. (See Figure 9.) One downside to the brace is the bulk and slippery external plastic, which causes issues with keeping the ankles together in a PLF position on landing. Lace-up supports were less effective at reducing the severity of ankle injuries but did decrease the number of them. Taping has shown similar reductions in injury frequency in both first-time and recurrent ankle sprains. Choosing which to use generally comes down to 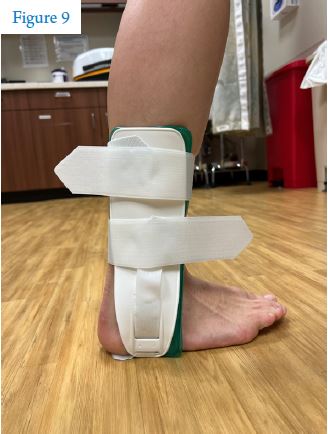 practical usability and cost. Ace wraps don’t have enough data to support their use in injury prevention. The most important factor appears to be simply wearing proper footwear. Loose-fitting, unstable shoes like flip-flops or Crocs will greatly increase injury risk compared to sneakers or well-fitted laced shoes.
practical usability and cost. Ace wraps don’t have enough data to support their use in injury prevention. The most important factor appears to be simply wearing proper footwear. Loose-fitting, unstable shoes like flip-flops or Crocs will greatly increase injury risk compared to sneakers or well-fitted laced shoes.
Regular physical training can also greatly decrease your chance of suffering an ankle injury. Avoid the weekend-warrior strategy, this just doesn’t work! Strengthening the supporting lower leg muscles, as well as balance and coordination training, will significantly reduce the risk of recurrent ankle sprains and injuries. Strengthening exercises include lunges, single-leg heel raises, elastic-band workouts with side-to-side shuffles and reverse lunges, and dips and squats. Balance training includes single-leg stands, star touches (as described above), and using tools like a wobble board or stability disc. Good stretching of your ankle before jumping can also help loosen stiff ligaments and tendons and prevent tearing or rupturing.
Last tip: Practice the movements of a good PLF with each reserve repack. When was the last time you practiced a PLF? Huh? Can’t hear you over there! Yeah … for most of us it would be the last time we helped teach a first-jump course or maybe even when we took our own first-jump course. This maneuver was designed to help prevent injury, and it really works when done correctly! How many of us have limped away (if we were lucky) from a face-plant landing that left us with more than just a bruised ego? If this maneuver becomes second nature, you have a higher chance of walking away from most dicey landings throughout your career.
Well, that wraps it up (so to speak) for ankle injuries. Next time, it’s all about knee injuries.
 About the Author
About the Author
Laura Galdamez, M.D., D-41824, began skydiving in early 2020. She works as an emergency medicine physician in Houston, Texas; is a Fellow of the Academy of Wilderness Medicine; and worked on the medical team for StratEx high-altitude balloon mission. She competes on several formation skydiving teams based at Skydive Arizona in Eloy.